Diseases once considered all but eradicated in the United States have re-emerged in the past several years. The resurgence of diseases like pertussis, tuberculosis, measles and mumps is an expression of the dangers posed by failing infrastructure and declining living standards for the working class.
According to the Centers for Disease Control and Prevention (CDC), pertussis (also known as “whooping cough”) is on the rise in states like California, Michigan and Ohio. Pertussis starts with symptoms similar to the common cold. The symptomatic similarity to the cold makes it hard to diagnose.
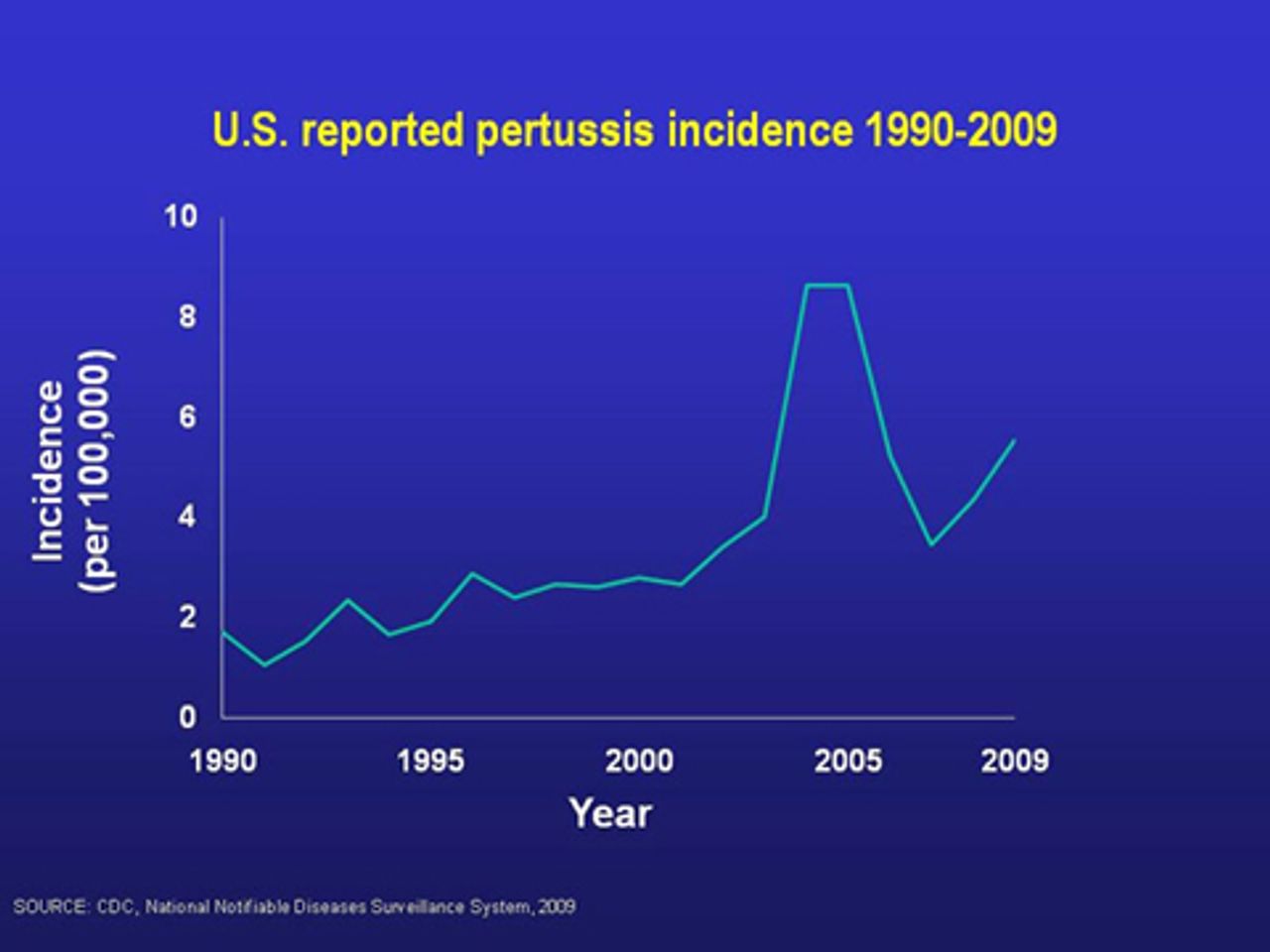
The difficulty in diagnosis in the early phases of the disease renders treatment with antibiotics useless for treatment of symptoms and prevention alike because the disease is most contagious in the first few weeks of infection. After a period of 1-2 weeks, it exacerbates into severe cough, and fits of coughing can be so severe that the victim vomits and succumbs to exhaustion. Coughing fits can also lead to rib fracture, loss of consciousness, incontinence, encephalopathy, pneumonia and death. Victims are subjected to these risks for six weeks or more.
From January 1 to December 31 in 2010, the CDC reported 8,383 confirmed cases of pertussis in California, which once enjoyed a living standard among the highest in the world. More than 1,100 adults and children have been diagnosed with the illness in San Diego County alone, and across the state at least 10 babies died. California has not suffered this great an outbreak since 1947.
Michigan, once home to a thriving auto industry, also suffered an increase in pertussis in the first half of 2008, continuing through 2010. There were 315 reported cases in 2008, with 902 cases in 2009 and 1,092 in 2010. Ohio recorded a level of infection not seen since 1985, with 966 reported cases.
The official figures do not include those who are unable to seek medical attention due to financial hardship. Given that the US is in the midst of the greatest economic crisis since the Great Depression and tens of millions lack health insurance, the real numbers are certainly much higher.
The denial of proper health care services in the first few weeks of pertussis infection leaves little doubt that the disease will spread through hospitals, schools, workplaces and other public settings. The limited nature of data collection caused by the neglect of the nation’s most vulnerable is doubly concerning.
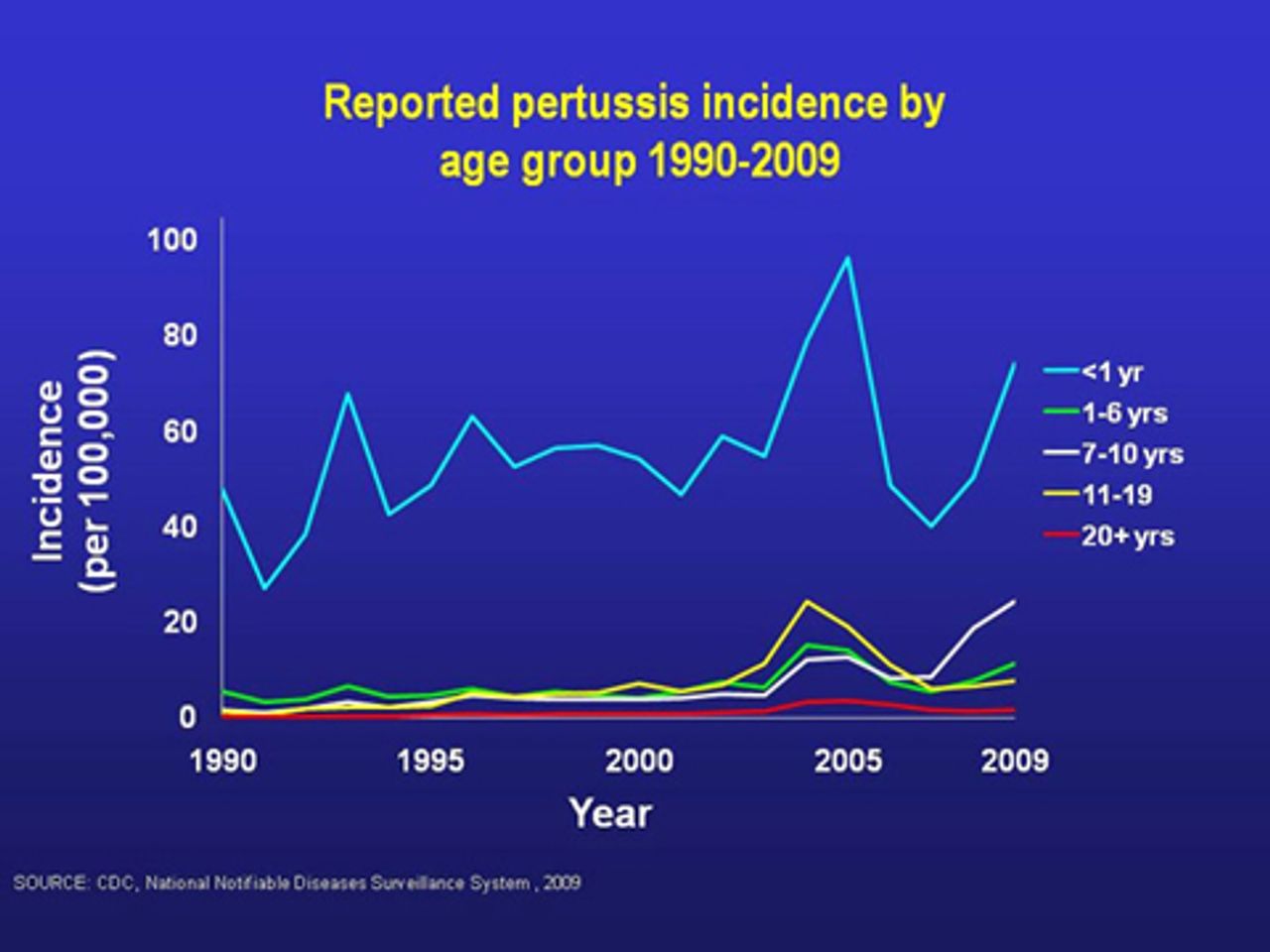
More disturbing are national levels of confirmed pertussis infection by age group. The CDC reports that infants aged six months or younger are at the greatest risk for severe disease and death. There was a 60 percent increase in incidence observed among this age group from 2008 to 2010. The incidence of the disease in adults 20 or younger was up by 40 percent in 2009.
Perhaps most telling is the rising incidence of diagnosed children aged 7 to 10. Cases among this age group saw a 9 percent rise in 2006, a 13 percent rise in 2007, a 23.5 percent rise in 2008, and a 23 percent rise in 2009.
Pertussis is easily preventable with the so-called “Tdap” vaccination, which protects against tetanus, pertussis and diphtheria. It was developed in the early 1920s and later perfected by Dr. Louis W. Sawyer. This vaccine led to almost complete eradication in the 1980s, but for it to be effective, a booster shot is necessary every 5-10 years. A deteriorating health care system, combined with the lack of any systematic monitoring of vaccinations nationwide, means that many people never get the necessary boosters.
Measles is a highly contagious viral disease that is spread through the air by small droplets. The year 2008 witnessed an outbreak of measles not seen since 1996, when a high percentage of cases were “imported.” By comparison, among the 131 cases diagnosed by July 2008, only 17 had been transmitted outside the US.
In all, 90 percent of those infected with measles in 2008 had not been vaccinated for the illness. With its high level of communicability and deadly complications, including pneumonia and encephalitis (swelling of the brain), one must ask why, in the wealthiest country in the world, measles still poses a significant health risk, especially among children.
Mumps is on the rise as well. In 2006, an outbreak mostly concentrated at colleges in the Midwest caused 6,584 cases. Mumps registered declines in 2007 and 2008, only to resurge in 2009 with a significant outbreak. Between August 2009 and February 2010, more than 1,000 people in New York and New Jersey were diagnosed with the mumps, a disease previously projected to be eliminated by 2010. Most of those afflicted had been vaccinated.
Tuberculosis, caused by bacteria and spread through the air, is also making a comeback, particularly among some segments of the working class population. In 2009, there were 11,545 reported cases of tuberculosis in the US, 29 percent of these among Hispanics. States with large immigrant populations have the highest incidence of tuberculosis. In 2009, there were 2,470 cases in California, 1,501 cases in Texas, and 1,006 cases in New York.
Tuberculosis is endemic to many parts of Mexico, specifically the northern states, due in large part to the failing infrastructure of the country and its poor public health services. The New York Times reports that immigration from Mexico to the US rose to more than 500,000 a year compared to less than 400,000 a year in the early 1990s. Thus, the worsening exploitation and social breakdown in Mexico are significant contributing factors to the rise of tuberculosis in the US.
The cholera outbreak in Haiti, which has killed more than 3,000 people and made over 100,000 Haitians severely sick, is a stark reminder of the importance of safe food and water supplies. Cholera is a food/water-borne illness that causes profuse diarrhea and, if not treated, can lead quickly to death.
On January 29, health officials in Massachusetts announced that six residents had tested positive for cholera after attending a wedding in the Dominican Republic and eating lobster brought from a town along Haiti’s border. Venezuela saw an eruption of 111 cases from the incident, along with at least 12 stricken with the disease in the Dominican Republic. Experts with the Dominican Medical Association have raised concerns that the national government is deliberately downplaying cholera rates in the country.
The United States has among the safest drinking water in the world, but funding cuts to public infrastructure, deregulation of government oversight, and the decay of the country’s water and sewage lines make potential food- or water-borne outbreaks more and more likely.
Some 48 million people suffer from food poisoning in the United States each year. Among those affected, 120,000 are hospitalized and 3,000 die. According to the CDC, approximately 90 percent of food-related illnesses, hospitalizations, and deaths were due to seven pathogens: Salmonella, norovirus, Campylobacter, Toxoplasma, E.coli O157, Listeria and Clostridium perfringens.
In 1993, the United States suffered the worst episode of water-borne disease with the outbreak of Cryptosporidiosis in Milwaukee, Wisconsin. Cryptosporidiosis is a parasitic disease caused by the protozoa Cryptosporidium parvum. Cryptosporidiosis infected more than 400,000 people between March 23 and April 8, 1993, and 54 died from the illness.
The rise of diseases long thought to be largely eradicated in the US should give the working class cause for concern. The resurgence of measles, mumps and pertussis demonstrates that the for-profit health care system is incompatible with health needs. The recent outbreaks of tuberculosis and cholera also indicate that a national approach is inadequate in fighting such diseases.
With further cuts to federal, state and local public health services on the agenda, there is little doubt that it is just a matter of time before another water- or food-borne illness creates a new health crisis.
